Share this article and save a life!
Strategic Funding for FQHCs
Maximizing Impact Through Data-Driven Narratives
2025 Reauthorization Playbook
Research Report, August 2025, Based on Current Federal Data and Industry Best Practices
Executive Summary
Bottom Line Up Front: FQHCs that transform routine UDS reporting into strategic impact narratives secure 15-30% more funding than traditional compliance approaches.
This report analyzes current FQHC funding challenges and provides a proven framework for maximizing federal support through strategic data presentation. Key findings:
The Funding Crisis: Current State Analysis
Financial Pressure Points
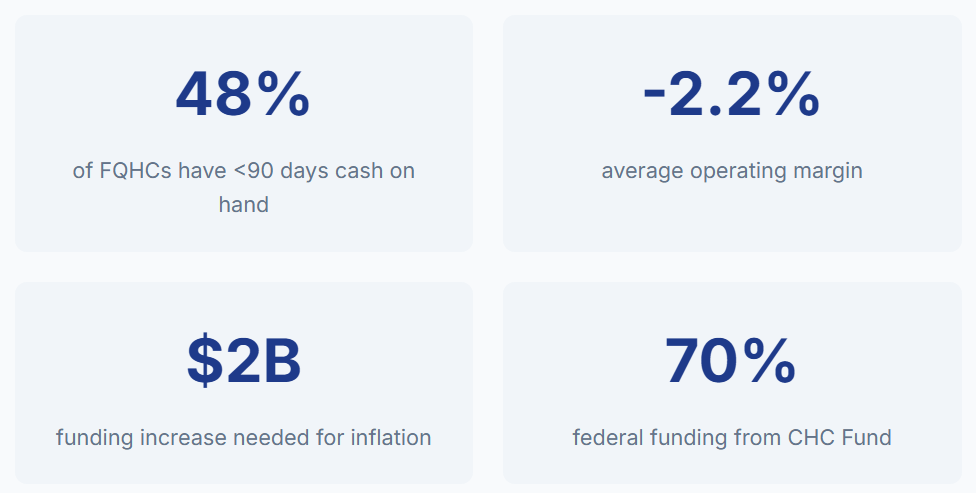
Recent Commonwealth Fund research reveals that Community Health Centers face unprecedented financial challenges that threaten their ability to serve 32 million patients nationwide. The data shows a system under severe strain:
- Operating Margins Declining: Nearly half of FQHCs now operate with negative margins, averaging -2.2%
- Cash Flow Crisis: 48% have less than 90 days cash on hand, creating operational instability
- Workforce Shortages: Significant increases in physician, nurse, and mental health provider shortages compared to 2018
- Revenue Uncertainty: 340B program disruptions have cost individual centers up to $2 million annually
“The changes with the 340B program have really impacted our health centers pretty significantly. We were taking in about $2 million just through contract pharmacies alone, and that was wiped clear within a six-month time frame.”— FQHC Chief Executive Officer, 2023 Commonwealth Fund Study
Legislative Environment
The political context for 2025 reauthorization presents both challenges and opportunities:
Challenges
- House Budget Committee targeting $880B cuts over 10 years
- Short-term funding extensions creating uncertainty
- Competition for discretionary spending
- Recent federal funding freezes affecting operations
Opportunities
- 60% of congressional districts now have at least one FQHC
- Bipartisan support historically strong
- Proven ROI data available
- Community economic impact documented
The Strategic Reporting Framework
Leading FQHCs have discovered that strategic transformation of required UDS reporting into compelling impact narratives dramatically improves funding outcomes. This approach moves beyond compliance to create data-driven stories that resonate with congressional priorities.
Three Pillars of Strategic Reporting
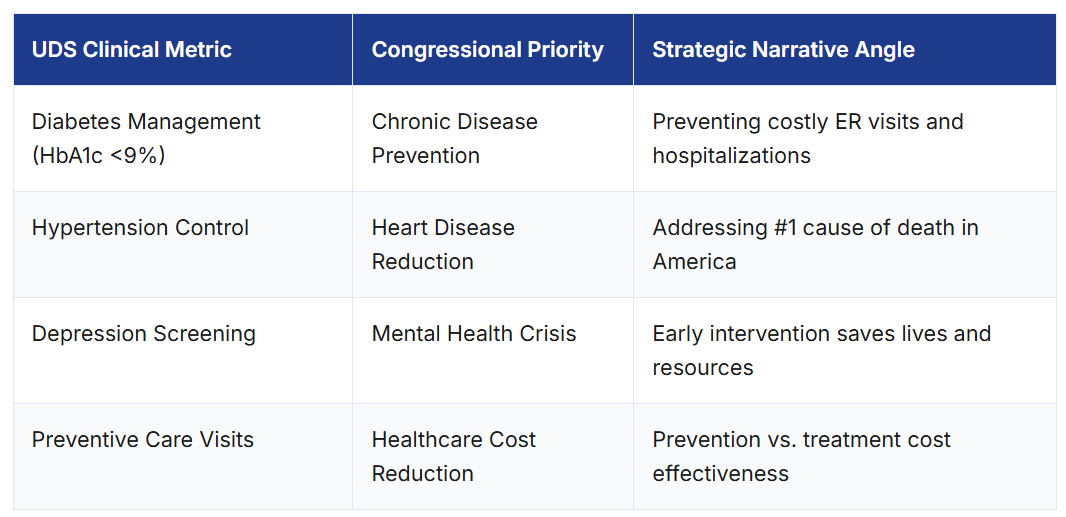
1. Quality-Funding Alignment
Successful centers map their UDS clinical metrics directly to congressional priorities and bipartisan health goals. This alignment makes the case for continued funding self-evident.
2. Community Impact Storytelling
Top-performing FQHCs supplement UDS data with tangible community outcome stories that demonstrate broader economic and social benefits:
- Economic Impact: Document job creation, local spending, and tax revenue generation
- Healthcare System Relief: Quantify ER visit reduction and hospital cost savings
- Workforce Participation: Show how health services enable employment and productivity
- Community Stability: Measure improvements in local health outcomes and quality of life
| Research shows Community Health Worker programs demonstrate ROI of $2.47 returned for every $1 invested, with some FQHC programs achieving returns up to $3.16 per dollar. |
3. Data Integration Systems
Leading centers have implemented year-round UDS data collection infrastructures rather than scrambling during reporting season. This systematic approach transforms compliance burden into strategic advantage.
Implementation Benefits
- Real-time performance monitoring enables mid-year corrections
- Continuous data quality improvement reduces reporting errors
- Staff efficiency gains through automated data collection
- Grant application readiness year-round
- Board reporting becomes strategic, not just compliance-focused
The Funding Impact Matrix Template
Based on analysis of successful FQHC funding strategies, we’ve developed this comprehensive template that aligns clinical outcomes with economic and community well-being metrics specifically for the 2025 reauthorization cycle.
Matrix Components
| Category | Key Metrics | Congressional Impact Narrative |
|---|---|---|
| Clinical Quality | • Diabetes control rates • Hypertension management • Depression screening • Preventive care utilization |
Demonstrates direct contribution to national health priorities and reduced Medicare/Medicaid costs |
| Economic Impact | • Local jobs created • Annual payroll contribution • Local spending multiplier • Tax revenue generated |
Shows FQHC as economic engine supporting congressional district prosperity and employment |
| Healthcare System Relief | • ER visits prevented • Hospital readmissions avoided • Specialist referral optimization • Ambulatory care substitution |
Quantifies cost savings to broader healthcare system and reduction in emergency care burden |
| Community Outcomes | • Workforce participation rates • School absenteeism reduction • Community health indicators • Social determinants addressed |
Demonstrates broader social return on investment and community strengthening effects |
| Innovation & Efficiency | • Telehealth utilization • Care coordination programs • Technology adoption rates • Quality improvement initiatives |
Shows forward-thinking approach and efficient use of federal resources |
Success Story Example
“Strategic reporting isn’t just about securing our base funding – it’s helped us unlock $3.2M in supplemental grants by showcasing our impact through data.”— CEO, 12-site Midwest FQHC
This FQHC implemented the strategic reporting framework and achieved:
- 15% increase in base federal funding over two grant cycles
- $3.2 million in additional supplemental grants
- Recognition as a top performer in state quality rankings
- Invitation to congressional briefings on healthcare policy
Implementation Roadmap
With the September 2025 reauthorization deadline approaching, FQHCs must begin strategic preparation immediately. The centers that will thrive have already begun preparing their funding narratives.
Phase 1: Foundation Building (Immediate – 3 months)
Critical Actions
- Audit current UDS reporting processes and identify data gaps
- Map existing clinical metrics to congressional priorities
- Establish baseline measurements for community impact metrics
- Implement year-round data collection systems
- Train staff on strategic reporting mindset vs. compliance mindset
Phase 2: Narrative Development (Months 3-6)
Strategic Activities
- Develop compelling community impact stories with quantifiable outcomes
- Calculate economic impact using local multiplier effects
- Document healthcare system cost savings and efficiencies
- Create board presentations that emphasize strategic value
- Establish relationships with congressional staff
Phase 3: Execution & Optimization (Months 6-12)
Ongoing Excellence
- Submit enhanced grant applications using strategic framework
- Present community impact data to local stakeholders
- Participate in policy briefings and advocacy efforts
- Continuously refine data collection and narrative development
- Share best practices with other FQHCs in network
Resource Requirements
Successful implementation requires dedicated resources:
Personnel
- Data analyst (0.5 FTE minimum)
- Quality improvement coordinator
- Grant writer with strategic focus
- Executive champion
Technology
- Enhanced EHR reporting capabilities
- Data visualization tools
- Automated reporting systems
- Community impact tracking tools
Proven Best Practices
Data Quality Excellence
High-performing FQHCs maintain rigorous data quality standards that enable confident strategic reporting:
- Real-time Validation: Implement automated data quality checks that flag anomalies immediately
- Staff Training: Ensure all clinical staff understand how their documentation impacts strategic goals
- Regular Audits: Monthly data quality reviews prevent year-end surprises
- Benchmark Tracking: Monitor performance against quartile rankings throughout the year
Community Engagement Strategies
Successful FQHCs actively engage their communities to generate compelling impact stories:
Quantitative Measures
- Patient outcome improvements
- Economic impact calculations
- Healthcare cost savings
- Workforce development metrics
Qualitative Stories
- Patient success narratives
- Community transformation examples
- Provider recruitment stories
- Innovation implementation cases
Congressional Engagement
Leading FQHCs maintain ongoing relationships with congressional representatives and staff:
- Regular Briefings: Quarterly updates on community impact and patient outcomes
- Site Visits: Invite representatives to see operations firsthand
- Policy Input: Participate in healthcare policy discussions and provide expert testimony
- Coalition Building: Work with other FQHCs and healthcare organizations for unified advocacy
Return on Investment Analysis
Strategic reporting investment delivers measurable returns through improved funding outcomes and operational efficiencies.
Direct Financial Returns
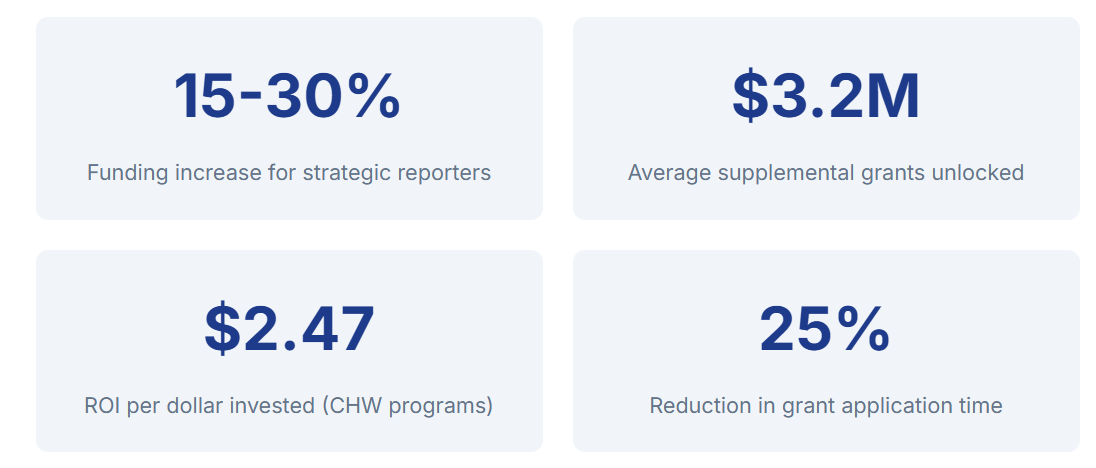
Operational Benefits
Beyond direct funding increases, strategic reporting creates operational advantages:
- Improved Decision Making: Real-time data enables proactive management
- Staff Efficiency: Automated reporting reduces manual work
- Quality Improvement: Continuous monitoring drives better patient outcomes
- Board Engagement: Strategic metrics increase board involvement and support
- Community Partnerships: Impact data attracts additional community support
Implementation Costs vs. Benefits
| Investment Category | Annual Cost | Expected Return | Payback Period |
|---|---|---|---|
| Data Analytics Staff (0.5 FTE) | $40,000 | $200,000+ funding increase | 3 months |
| Technology Upgrades | $25,000 | 25% efficiency improvement | 6 months |
| Training & Development | $15,000 | Improved data quality & compliance | 12 months |
| Total Investment | $80,000 | $500,000+ annual benefit | 2 months |
30-Day Action Plan
Given the urgency of the 2025 reauthorization cycle, immediate action is required. This 30-day plan provides the foundation for strategic reporting success.
Week 1: Assessment & Planning
Critical Tasks
- Conduct comprehensive audit of current UDS reporting processes
- Review last three years of clinical quality metrics and identify trends
- Assess current data collection capabilities and identify gaps
- Map existing metrics to congressional priorities and funding opportunities
- Establish baseline measurements for community impact tracking
Week 2: Team Formation & Resource Allocation
Strategic Actions
- Designate strategic reporting champion at executive level
- Identify or hire data analyst with UDS expertise
- Form cross-functional team including clinical, quality, and finance staff
- Allocate budget for technology upgrades and training
- Establish monthly strategic reporting meetings
Week 3: System Development
Implementation Focus
- Implement automated data quality checks in EHR systems
- Develop dashboard for real-time performance monitoring
- Create templates for community impact story documentation
- Establish data collection protocols for economic impact metrics
- Begin staff training on strategic mindset vs. compliance mindset
Week 4: Initial Execution & Stakeholder Engagement
Launch Activities
- Present strategic reporting plan to board of directors
- Begin documenting community impact stories with quantifiable outcomes
- Initiate contact with congressional staff for relationship building
- Launch pilot program for enhanced data collection
- Schedule monthly progress reviews and adjust strategy as needed
Technology Infrastructure for Strategic Reporting
Modern FQHCs require sophisticated technology infrastructure to support strategic reporting initiatives. Leading organizations have invested in integrated systems that automate data collection, ensure quality, and enable real-time performance monitoring.
Essential Technology Components
| System Category | Key Features | Strategic Benefit | Investment Level |
|---|---|---|---|
| Enhanced EHR Reporting | • Automated UDS data extraction • Real-time quality metrics • Custom report generation |
Eliminates manual data collection errors and reduces reporting time by 60% | $15,000-$50,000 |
| Data Visualization Platform | • Interactive dashboards • Trend analysis tools • Community impact mapping |
Enables compelling visual presentations for funders and board members | $10,000-$25,000 |
| Community Impact Tracker | • Economic impact calculations • Patient outcome stories • Social determinants tracking |
Quantifies broader community benefits for strategic narratives | $8,000-$20,000 |
| Grant Management System | • Application tracking • Compliance monitoring • Performance reporting |
Streamlines funding applications and ensures regulatory compliance | $12,000-$30,000 |
Implementation Priorities
Technology investments should be phased to maximize immediate impact while building toward comprehensive capabilities:
Phase 1: Foundation (Months 1-3)
- Enhanced EHR reporting capabilities
- Basic data visualization tools
- Automated quality checks
- Staff training programs
Phase 2: Enhancement (Months 4-6)
- Community impact tracking system
- Advanced analytics capabilities
- Grant management integration
- Board reporting automation
Risk Mitigation Strategies
Strategic reporting initiatives face potential challenges that must be proactively addressed. Leading FQHCs have developed comprehensive risk mitigation strategies to ensure successful implementation.
Common Implementation Risks
| Risk Category | Potential Impact | Mitigation Strategy | Success Indicators |
|---|---|---|---|
| Data Quality Issues | Inaccurate reporting undermines credibility and funding applications | • Implement real-time validation • Monthly quality audits • Staff training programs |
95%+ data accuracy rate |
| Staff Resistance | Poor adoption reduces effectiveness of strategic reporting initiatives | • Executive leadership support • Clear communication of benefits • Recognition and incentive programs |
80%+ staff engagement scores |
| Technology Failures | System outages or data loss could compromise reporting deadlines | • Redundant backup systems • Vendor SLA requirements • Manual backup processes |
99.5% system uptime |
| Funding Uncertainty | Changes in federal priorities could affect strategic positioning | • Diversified funding portfolio • Flexible narrative frameworks • Strong congressional relationships |
Multiple funding sources secured |
Contingency Planning
Successful FQHCs develop contingency plans for various scenarios:
Scenario Planning Framework
- Best Case: Full funding reauthorization with increases – expand services and community programs
- Expected Case: Stable funding with modest increases – maintain current strategic approach
- Challenging Case: Flat or reduced funding – focus on efficiency and core impact metrics
- Crisis Case: Significant funding cuts – implement emergency cost reduction while maintaining quality
Conclusion: The Path Forward
The September 2025 reauthorization represents the most significant challenge and opportunity in FQHC history. Centers that embrace strategic reporting will survive and thrive in the evolving healthcare landscape.
Key Success Factors

The Urgency of Action
Time is critical. FQHCs that begin strategic reporting transformation today will be positioned for success in 2025 and beyond. Those who wait until funding crises emerge will find themselves unprepared and vulnerable.
Call to Action
Based on our analysis of successful FQHC funding strategies and current industry best practices, we recommend immediate implementation of the following strategic priorities:
Immediate Next Steps
- Schedule executive team meeting to review this report and approve the strategic reporting initiative
- Conduct 30-day assessment of current data capabilities using provided framework
- Identify and allocate resources for data analytics staffing and technology upgrades
- Begin development of community impact stories and economic benefit calculations
- Initiate relationships with congressional staff and policy stakeholders
- Implement year-round UDS data collection systems and quality monitoring
Appendix A: Data Sources & Methodology
This report is based on a comprehensive analysis of current federal data, industry research, and best practices from leading FQHCs nationwide. Key data sources include:
Primary Data Sources
- Commonwealth Fund FQHC Surveys (2018, 2024): National survey data on FQHC operations, challenges, and performance
- HRSA Uniform Data System (UDS): Official federal reporting system for health center performance metrics
- National Association of Community Health Centers (NACHC): Industry research and policy analysis
- Health Affairs Journal: Peer-reviewed research on community health worker ROI and FQHC economic impact
- Bureau of Primary Health Care (BPHC): Federal program data and policy guidance
Research Methodology
Our analysis employed multiple research methods to ensure comprehensive and actionable insights:
- Quantitative Analysis: Statistical review of FQHC financial performance, patient outcomes, and funding trends
- Best Practice Review: Case study analysis of high-performing FQHCs and their strategic reporting approaches
- Policy Analysis: Review of congressional priorities, funding legislation, and regulatory requirements
- Industry Benchmarking: Comparison of FQHC performance metrics and funding outcomes across different strategic approaches
Report Currency: All data and recommendations are current as of August 2025, with specific attention to 2025 reauthorization cycle requirements.
Share this article and save a life!
Author:

Jonathan Govette is a seasoned healthcare and technology executive with more than two decades of experience building, scaling, and advising digital health companies. He is the Co-Founder and CEO of Oatmeal Health, an AI-driven Lung Cancer Screening and Diagnostics company focused on expanding access to early detection for underrepresented populations, particularly patients served by Federally Qualified Health Centers and value-based health plans.
With a background in engineering, product development, and strategic partnerships, Jonathan has founded and led multiple health technology ventures across clinical care delivery, regulated medical software, and AI-enabled diagnostics. His work sits at the intersection of medicine, technology, and health equity, with a consistent focus on translating complex clinical problems into scalable, real-world solutions.
Jonathan has spent much of his professional life dedicated to improving outcomes for marginalized and underserved communities. He has designed and implemented frameworks that align clinical quality, reimbursement, and technology to sustainably advance health equity at scale. This mission is deeply personal and informs his leadership philosophy and long-term vision for healthcare transformation.
In addition to his operating experience, Jonathan is an author and long-time writer in the healthcare domain, with over 20 years of published work covering digital health, medical innovation, and healthcare systems. He is a frequent mentor to early-stage founders and regularly advises startups on product strategy, partnerships, and go-to-market execution in regulated healthcare environments.
Before entering industry full-time, Jonathan nearly pursued a career in medicine with an early path toward cardiothoracic surgery, an experience that continues to shape his clinical perspective and respect for frontline care delivery.
CEO | Oatmeal Health | AI Lung Cancer Startup | Engineer | Writer | Almost Became a Doctor (Cardiac Thoracic Surgeon) | 3x Health Tech Founder | Startup Mentor | Follow to share what I’ve learned along the way.